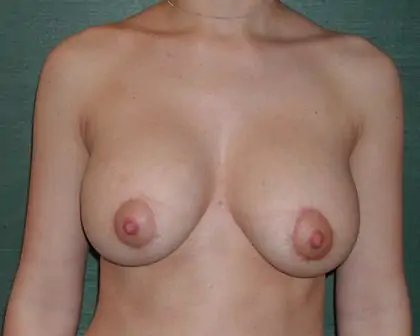
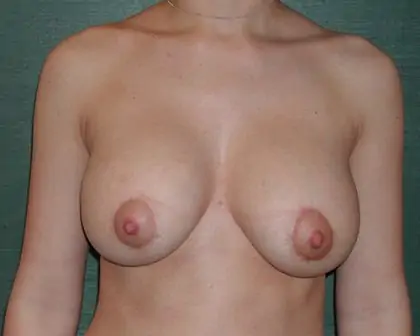
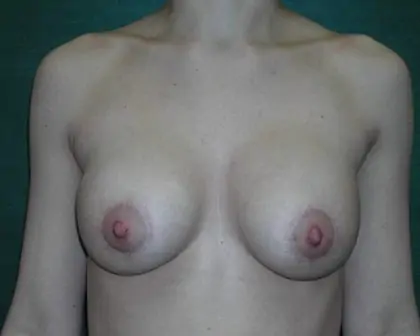
Breast implant surgery and revision techniques can vary from something as simple as removing or exchanging one or both implants, to modifying the breast pocket, to removal or repair of the scar tissue that forms the capsule around silicone and saline breast implants.
Contents
showCandidates
A good candidate is a person who desires a change or improvement to the breast after their previous breast surgery and is otherwise healthy. If a person is deemed medically fit for prior breast surgery, they are almost always still well-qualified for revision procedures.
The qualifications and requirements of breast revision surgery will likely be very similar to the previous surgery to enhance the breasts, including avoiding certain medications and supplements for a given period prior to the treatment.
Consultation
During the consultation with board-certified plastic surgeon Dr. Steven Wallach, you will spend a lot of time reviewing your breast revision surgery goals. An exam will then be performed and a plastic surgery plan to address your unique concerns revision surgery will be discussed with you at length.
You can also use this time to ask Dr. Wallach any questions you may have about the procedure and what results you can expect. For those disappointed with their initial results, it’s not uncommon to feel apprehensive about continuing to undergo breast revision surgeries, which is why we work hard to understand your motivations, expectations, and worries prior to committing to a surgery date.
Preparation
You should ask your New York plastic surgeon if they are board-certified first and foremost, as you should not entrust this procedure to someone who isn’t committed to the same ethical and professional standards that board-certified physicians are. You might want to review the various plastic surgery techniques as well and which breast revision surgery technique they feel will give you the best result with the least amount of scarring.
Patients may choose to change from saline implants to silicone implants, wish a change in the implant size, or want complete implant removal during their revision procedure. Your consultation with Dr. Wallach provides you the ability to discuss all your aesthetic goals and determine the best breast revision surgery technique that will help you achieve them.
Testimonials
Risks
The main risks of breast implant revision surgery are unfavorable scarring, asymmetry, infection, bleeding, nipple loss, skin loss, fat necrosis, fluid collections, implant issues, numbness or hypersensitivity, and the need for further breast revision surgery.
Recovery
Most patients can go back to light-duty work within 3-5 days. Pain and discomfort are minimal depending on the technique used and goals achieved from surgery. Dr. Wallach has patients avoid strenuous activity for 3-4 weeks and then avoid exertion like heavy lifting for about 6-8 weeks to ensure everything heals correctly.
Patients may have many reasons for choosing to undergo revision breast procedures but the goal of the breast revision surgery in New York is to improve the appearance of your breasts and give you natural-looking results.
Find The Best Treatment For You
Explore Our Procedures
Common Reasons for Breast Revision
There are many reasons both medical and aesthetic for choosing to pursue breast revision surgery. Common medical reasons include capsular contracture, implant rupture, or other conditions that cause pain. There are also legitimate aesthetic reasons to seek revision breast surgery, including rippling, unpleasing placement or deformity, and changes in appearance with movement.
ANIMATION DEFORMITIES
When saline or silicone implants are placed in a submuscular pocket, sometimes patients have animation deformities of the breasts. The implant can appear to move upward and toward the axilla, and a ridge can sometimes be seen at the juncture between the lower muscle border and the breast tissue. This can be the result of over-release of the medial muscle fibers along the sternum, or simply with wear and tear with thin soft tissue coverage.
The revision procedure for this may include moving the implant into a subglandular pocket, adding an ADM (Acellular Dermal Matrix) such as Strattice® (LifeCell) to the lower pole, releasing the muscle from the gland, or performing a split-muscle technique.
BOTTOMING OUT
“Bottoming out” refers to the situation when a silicone or saline implant descends below the inframammary fold of the breast. This can happen as a result of over-dissection of the implant pocket, having a tuberous breast deformity, or over time as the implant pushes below the fold
In this situation, the nipple may be pointing upward, and usually the majority of the implants may fall below the horizontal line of the nipple and around the areola. Revision procedure for this deformity will require possible implant removal for exchange with a smaller implant, a capsulorrhaphy (capsule repair), and/or inserting an ADM for further support along the lower pole.
CAPSULAR CONTRACTURE
The body forms a natural barrier of tissue around all new implants in the body, including breast implants. When this barrier gets tight around the implant causing deformity and pain, this is called a contracture. Clinically, patients may find the breast to be painful and the implant will not move freely in the pocket. When this happens, the silicone gel or saline implant tends to sit higher on the chest than intended.
Breast revision treatment often requires removal and exchange of the implants, sometimes including a change in the pocket position from subglandular to submuscular or vice versa, removal of the capsule, and possibly inserting an ADM such as Strattice (LifeCell).
“Beauty is the internal light that emanates from within. To me, the true form of beauty is one’s personality that shines through.”
Steven Wallach, MD
DOUBLE BUBBLE DEFORMITY
A “double bubble” can be the result of several different scenarios, each requiring a different surgical technique to repair it. Common causes of a double bubble include: an implant that is too large for the breast, an implant that sits too high on the chest with the gland “falling off” the implant, a tight breast in the lower pole often seen with tuberous-looking breast, and from capsular contracture.
Correction of this problem is dependent on the cause. If the implant used during the initial breast augmentation is too large for the base diameter of the breast, a smaller implant can be used or the lower breast pole can be released by making radial cuts in the gland to expand around the implant. If the initial breast augmentation implant sits too high because of inadequate release of the pectoralis muscle, then the breast augmentation revision procedure will include releasing this muscle a bit more. If the breast is still “falling off” the implant, then plastic surgeons sometimes decide to perform a breast lift. If the breast is tuberous and the lower pole is tight, then radial cuts along the lower breast pole during breast revision can potentially improve this situation. If a contracture is causing the double bubble, then a capsule excision may help.
Of course, variations of all these breast augmentation revision techniques may be necessary to help you achieve the desired size, shape, and natural-looking results.
LATERALIZATION OF THE IMPLANTS
When the pocket becomes too large either from over-dissection or over time with tissue expansion, the initial breast implants can fall off to the sides when the person is lying down. Treatment of this deformity can be accomplished by performing a capsulorrhaphy (capsule tightening procedure) along the lateral chest wall. This may include the use of permanent or slowly resorbable sutures, reinforcing part of the capsule to itself, or reinforcing the repair with ADM such as Strattice (LifeCell).
All your breast augmentation revision procedures are performed under general anesthesia. During your consultation, NYC breast surgery Dr. Wallach will discuss the best options with you to help you get the breast enhancement you desire.
SYMMASTIA
This is essentially the opposite of lateralization of the implants. This is when the inside portions of the breast pocket were either over-dissected during surgery or due to stretching over time. In this case, the implant migrates toward the sternum and the cleavage becomes crowded or lost. This is more common with subglandular implant placement.
Correction of this deformity can be accomplished by a breast revision plastic surgery procedure that creates a submuscular pocket, or by performing a capsulorrhaphy, which can include reinforcing the capsule and/or inserting an ADM such as Strattice (LifeCell).
RIPPLING
Visibility of the implant through the skin after breast augmentation is often a sign of rippling. This is a result of the skin being too thin to cover the implant most often due to the patient being very thin or having undergone many previous breast enhancement surgeries. The goal of the revision breast surgery is to provide better soft tissue coverage over the implant if possible. If the implant is in a subglandular pocket, placing it in a submuscular pocket may help. In the case of a saline implant, sometimes over-filling the implant will remove the ridging of the implant and therefore improve the rippling.
Usually the goal of the revision breast surgery is to provide more soft tissue coverage, so fat grafting can sometimes be helpful, as well as inserting an ADM such as Strattice (LifeCell) over the implant in the rippling areas.
Schedule a Breast Revision Consultation
If you would like more information about New York City plastic surgeon Dr. Wallach and his success with New York City breast revision procedures, we hope that you will not hesitate to contact our Manhattan offices at (212) 861-6400 or by using our contact form to request additional details. Whether your problem is medical or simply cosmetic, we’re here to help you get the care you need with a highly personalized breast revision surgery that gives you the naturally beautiful results you wanted in the first place.
Video Library
Featured Videos
Explore real procedures, patient testimonials, and educational content from our expert medical team
FAQs
Can breast implants be removed and not replaced?
Can breast implants last 30 years?
Does insurance pay for breast implant revision?
How much is a breast implant revision?
What is breast revision surgery?
What is symmastia? And why does this happen?
I think my implant is moving toward the center of my chest and causing a symmastia. How can this be fixed?
Can breast implants change shape over time?
Can breast implants last a lifetime?
Can you feel a ruptured breast implant?
Does insurance cover breast revision?
How long do breast lifts last?
How often should breast implants be replaced?
Is it dangerous to have breast implants removed?
Is there an alternative to breast implants?
My breast implants cause pain. Does this mean I have a capsular contracture?
What is a capsular contracture?
How does one treat a capsular contracture?
I am unhappy with the implants that were placed and I want bigger ones. When can I get a revision?
I think I have bottoming out of my implants. How does one get this fixed?
My implant shape looks funny. How is it fixed?
Can I have my breast implants removed?
Can breast implants be reduced in size?
Can capsular contracture get worse?
Can capsular contracture go away by itself?
How do you fix capsular contracture?
What are the early signs of capsular contracture?
I have a double bubble. What causes this?
I have a double bubble. How does this get fixed?
How long does it take to recover from breast revision surgery?
How soon after breast augmentation can I get a revision?
What is the most common breast implant size?
I have rippling of my implants. What causes this?
Should my implants be placed above or below the muscle?
What happens if I just remove my implants?
What happens if I want smaller implants because my implants are too big?
My implant seems to move into my armpit. What do I do?
Dr. Steven Wallach is a board-certified plastic surgeon in New York City specializing in aesthetic facial and body contouring, as well as reconstructive surgery. With more than 25 years in practice and over 15,000 surgeries performed, he brings extensive experience and refined surgical skill to every procedure. He earned his medical degree from NYU School of Medicine and completed advanced training at Albert Einstein College of Medicine/Montefiore Medical Center, followed by a prestigious fellowship in California. A past president of the New York Regional Society of Plastic Surgeons and former executive board member of The Aesthetic Society, Dr. Wallach is frequently recognized for his expertise, including in New York Magazine’s “Best Beauty Docs.” In addition to his clinical practice, he is an Associate Clinical Professor at Albert Einstein and regularly contributes to medical publications and national media. Known for his innovative techniques and compassionate care, he helps patients achieve natural, confidence-boosting results.