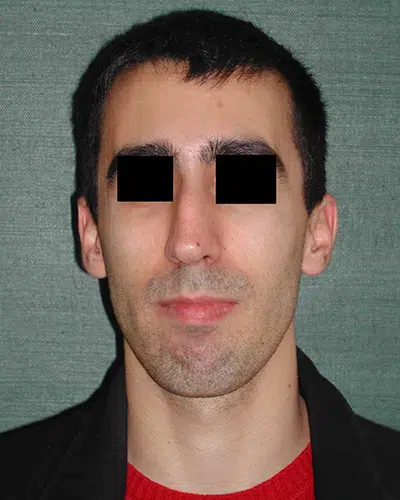
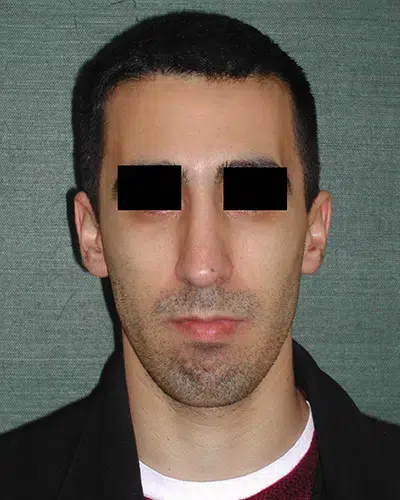
Patients undergo rhinoplasties to resolve common sources of aesthetic dissatisfaction, such as a prominent dorsal hump, asymmetrical nasal contours, and the size, shape, and position of the nasal tip. Other patients may have difficulty breathing as the result of a deviated septum or an injury. Regardless of their motivation, with today’s advanced approaches to rhinoplasty, and in the hands of a talented and experienced plastic surgeon, today’s patients can avoid the unfortunate “cookie-cutter” nose of years past.
Dr. Steven Wallach is a leading expert in plastic and reconstructive surgery. He is frequently consulted by major beauty publications and national medical and academic institutions alike. As one of the top board-certified plastic surgeons in New York City, he is renowned for consistently delivering outstanding results that are carefully tailored to each patient. Schedule an initial consultation today. You can reach his 5th Avenue offices directly by calling (212) 861-6400, or by filling out an online contact form at your convenience.
Contents
showAbout
Our nose starts developing in the 10th week after conception and continues to take shape until we’re in our teens. [1] However, whether as a result of genetics or sustained injuries, both the form and function of this prominent facial feature can present troubling concerns. Whether patients are struggling with breathing issues or are unhappy with their appearance, a rhinoplasty can help.
Rhinoplasty is one of the most commonly performed plastic surgeries, and today’s approaches to this procedure preserve the integrity of the inner structure of the nose. As a result, patients enjoy an easier recovery, a lower risk of complications requiring revisions, and results that can be tailored to their unique anatomy and desires. During surgery, a surgeon adjusts the underlying cartilage, bone, and soft tissue to correct aesthetic and functional concerns. [2] The nose is an incredibly complex organ, and when considering a rhinoplasty, it’s essential to choose an experienced plastic surgeon that is sensitive to the patient’s desires while also realistic about the changes that can be safely achieved. Dr. Wallach frequently resolves breathing issues while also addressing a patient’s aesthetic concerns for balanced, natural-looking results and improved airflow.
Cosmetic Rhinoplasty Approaches
ETHNIC RHINOPLASTY
Dr. Wallach does not like this phrase because it is often used to describe select ethnic groups that undergo rhinoplasty. Dr. Wallach practices in New York City– his patients are of all ethnicities and commonly of mixed ethnicities. He feels that every patient is ethnically unique, and so in reality, every rhinoplasty is an “ethnic rhinoplasty.” His goal is always the same: for his patients to maintain their ethnic identity and yet give them a natural-looking result that fulfills their desires.
DORSAL HUMP
A common source of dismay, a prominent bridge of the nose, or dorsal hump is a frequent motivation for cosmetic rhinoplasty. This feature of the nose is formed by the meeting of the nasal bones and the upper lateral cartilage. In order to create a smoother nasal profile, surgeons often shave down sections of the nasal bones. To correct the flat plane that results from these modifications, and to achieve other structural alterations, surgeons perform an osteotomy. Osteotomies adjust the angling of the two nasal bones at the very top of the nose. The bones can be moved inward or outward to adjust the nasal width and restore a natural nasal shape. This can be done with several different types of bone cuts: low-to-high, low-to-low, medial oblique, or even double-level cuts. In some cases, especially after trauma, the bones sometimes need to be out-fractured to restore nasal width. Then, the remaining bone is readjusted to achieve a refined, natural-looking shape.
TIP REFINEMENT
Patients who wish to correct a bulbous, boxy, or wide nasal appearance can do so with a treatment that solely focuses on the tip of the nose. The lower lateral nasal cartilage is modified during surgery to improve tip projection. Some patients may have cartilage grafts as well to improve the tip contours.
Many patients desire improvement for the tip of their nose. Sometimes the tips are “boxy,” bulbous, rounded, clefted, or just unsatisfying. These deformities can be related to the underlying anatomical structures that create the tip: the lower lateral nasal cartilages. These mirror-image pieces of cartilage meet in the center of the tip of the nose and contribute to its appearance and angling. They can be modified with partial excision as well as with suturing techniques to create the desired shape. Sometimes, cartilage grafts are used to improve tip projection as well and are secured to the cartilage in the columella region.
The overlying skin envelope also contributes to the overall shape of the nasal tip. In patients with thicker skin, these underlying structures may not be as well-defined as in someone with very thin skin. The thicker skin and soft tissue envelope tend to blunt the underlying structures and hide them, therefore, thinning the subcutaneous tissue a bit may improve the tip definition.
ALAR BASE REDUCTION
Alar base reduction surgery is often requested in patients that have a wide nasal base and complain of flaring nostrils. A general guideline for evaluating the nostrils and the nasal base is to compare their relationship to a line drawn down from the inner portion of each eye.
There are several different types of alar base reduction procedures that excise various portions of the alar rim to reduce the flare of the nostril and/or the nasal width, and they are chosen based upon the given anatomy and patient goals. These procedures can be done at the same time as the rhinoplasty, but also can be done under local anesthesia at a later time.
Functional Concerns and Corrective Procedures
EXTERNAL VALVE COLLAPSE
This refers to the nostril valve, or the external and internal structures around the nasal rim, including the columella (the area of tissue between the nostrils), the lower lateral cartilage (LLC), and the nasal floor. This valve collapses upon inhalation and is usually due to weak LLC either from genetics, trauma, or previous rhinoplasties.[3] Usually, providing better support to the LLC will improve this condition. This can be accomplished with cartilage grafts sutured to the LLC or columella.
INTERNAL VALVE COLLAPSE
The internal nasal valves are located in the middle section of the nose. These valves are formed by the upper lateral cartilage (ULC), the nasal sidewall, the septum, and the inferior turbinate. Patients with internal valve collapse have visible depressions in the middle third of their nose when breathing deeply. Treatment of the collapse can be accomplished by placing a cartilage graft, commonly known as a spreader graft, between the septum and ULC. An alternative is to fold in a portion of the ULC as a graft to increase the angle between the ULC and septum. [4]
TURBINATE HYPERTROPHY
Turbinates are tiny structures in the nose made up of bone and mucosa that humidify the air. If they become enlarged, they may cause airflow obstruction. They can be removed or resected to rectify the problem and improve respiratory function.
DEVIATED SEPTUM
Breathing problems, snoring, nose bleeds, and chronic sinus problems can be caused by a curved septum. Treatment of the septal deviation can be done using suture techniques, scoring of the cartilage, reinforcement of the cartilage with grafts, and/or removal of a portion of the deviated cartilage as in a submucous resection (SMR). Commonly, an SMR procedure will provide cartilage graft material for use in other areas such as for spreader grafts, batten grafts to straighten the septum, alar cartilage grafts for support of the nasal rim, and as tip grafts, to name a few.
Grafting Options
Some treatments require cartilage grafting to correct the tip and overall nasal shape. Grafting can be accomplished using your tissue (an autologous graft) or with a synthetic graft.
AUTOLOGOUS GRAFTING CHOICES
- Ear Cartilage: An incision is made behind the ear, so a piece from the conchal bowl is harvested. This particular treatment is best utilized for tip grafting and spreader grafting. However, it does not have the same structural support as a septal or rib cartilage graft.
- Rib Cartilage: Rib cartilage is harvested from the chest wall. A small incision on the chest is used to obtain the graft, and in women, it is often harvested through a small incision under the breast fold. This usually provides the largest amount of graft material. It is commonly used when a significantly large dorsal augmentation is required for flat noses. It can be used for most other grafting requirements as well. The main drawback is the scar and the discomfort.
- Septal Cartilage: Septal cartilage is an excellent source of cartilage and can be molded for almost any use. It is often the first choice of graft material because the septum is very commonly exposed during rhinoplasty, and often treated for deviations during rhinoplasty. As a result, there are no additional external incisions required to harvest the graft.
- Temporalis Fascia: Temporalis fascia is found in the lateral forehead region within the hairline. Fascia is the soft, white connective tissue layer that covers muscle tissue in many different areas of the body. The incision used to harvest this particular fascia is hidden within the hairline. Temporalis fascia is often used for camouflage purposes when the overlying skin is very thin, so underlying structures are not as noticeable. It is also used for dorsal onlay procedures when diced cartilage is used for nasal augmentation.
NON-AUTOLOGOUS GRAFTING CHOICES
Non-autologous grafts can be synthetic or acquired from donor tissue.
- Acellular Dermal Matrix (ADM): ADMs are derived from dermis or skin elements that are treated to remove all antigenic material. They are from either human or porcine tissue. They are used in a similar fashion to the fascia. They are good for camouflage purposes to cover the framework structures under a thin skin envelope.
- Irradiated or non-irradiated Homograft Costal Cartilage (IHCC): This is rib cartilage that is harvested from a human cadaver and treated so that all antigenicity and any microorganisms are removed. This is used as a cartilage graft like those in the autologous cartilage graft descriptions. It is an excellent product that eliminates the harvest of the patient’s own rib cartilage, thus avoiding incision and discomfort. It is commonly used when multiple cartilage grafts are needed, when there are not enough donor site grafts available from the septum or ear, or when the patient does not want their own rib to be harvested. There have been several studies in the medical literature showing the long-term use and efficacy of this product.
- Synthetic Grafts: Gore-Tex, Porex, and silicone are all types of synthetic grafts that are available for nasal augmentation. Since they are synthetic and they do not become incorporated into the adjoining tissue, they have a higher incidence of infection and extrusion. [5] Dr. Wallach does not usually use these products for nasal grafting and prefers autologous tissue grafts when available.
Benefits
Rhinoplasty allows patients to have a direct influence on their nasal appearance and function. Patients receiving surgery can also look forward to:
- The ability to make corrections to the nasal shape, size, and symmetry
- Resolve breathing problems caused by blocked nasal passageways
- A customized treatment that can treat multiple nasal concerns
- Preserves ethnic and gender attributes
- A rise in self-confidence and esteem
Ideal Candidates
Healthy men and women concerned about their nasal appearance and respiratory function can experience significant improvement with rhinoplasty surgery. Your meeting with Dr. Wallach will determine if you’re a good candidate for surgery.
IDEAL RHINOPLASTY PATIENTS IN NEW YORK CITY
- Are self-conscious about their nasal appearance
- Wish to correct breathing problems
- Are girls at least 15 years old or boys that are 17 years old or have reached full maturity[1]
- Non-smokers or willing to quit using nicotine products leading up to their surgery and for the duration of their recovery
- Not involved in intranasal drug use such as cocaine [2]
Personal Consultation with Dr. Wallach
“As an expert in the field of plastic surgery, one of the most rewarding aspects of my career has been listening to my patients’ stories about how having plastic surgery has changed their lives.”
— Steven Wallach, MD
Your consultation is your opportunity to discuss the concerns you have with your nose and learn more about whether a rhinoplasty can achieve your goals. Dr. Wallach will listen closely, answer any questions that you may have, and examine your nose’s shape and structure to begin formulating a personalized treatment plan. We’ll also see if you meet the prerequisites for surgery by reviewing your medical history, including any past facial surgeries.
Book your appointment with us today by calling (212) 861-6400 or filling out an online contact form.
Preparation
Every patient will receive detailed instructions on how to prepare for surgery. Successful planning will ensure a worry-free experience and optimal results. Before your rhinoplasty:
- Stop using nicotine products several weeks before surgery.
- Fill prescriptions and acquire other recovery medications in advance.
- Discontinue certain medications, including NSAIDs, supplements, and blood thinners.
- Shop for soft foods to make eating easier after surgery.
- Arrange for a ride home by a trusted adult, or have them escort you if taking a car service.
Procedure
Depending on the complexity of your rhinoplasty surgery, you will be administered either sedation anesthesia, or general anesthesia, depending on your preferences and the complexity of your surgery. Once it has taken effect, Dr. Wallach will begin.
Rhinoplasties are performed using an open or closed surgical approach. Traditionally, the closed approach was the most common surgical incision technique used to gain access to the underlying nasal framework during surgery. This usually employed various internal incisions and could include incisions between the upper and lower lateral cartilages, at the inferior border of the lower lateral cartilages, or within the border of the lower lateral cartilages. Commonly, this was combined with a transfixion incision (along the lower border of the septum). This closed approach can be used in many instances, and some surgeons exclusively use closed rhinoplasty. However, many surgeons have moved away from this approach and now the open technique is the most popular approach..
The open approach also uses some or all of these previously described incisions but includes a small incision on the skin of the columella. The columella is the area between the two nostrils. The incision added is only about 0.5 -1 cm in length but allows much more exposure and visibility for the surgeon. Since the columella incision is concealed by the shadow of the nose, when looking at someone straight on, the columella incision is often well hidden. Most surgeons feel that with this better exposure, more precise and accurate work can be done. Dr. Wallach prefers this technique for most of his New York rhinoplasty patients. To learn more about open vs. closed rhinoplasty, take a look at one of Dr. Wallach’s blog posts.
Once Dr. Wallach has access to the underlying structure of the nose, he will perform the necessary alterations. Cartilage may be trimmed, sutured, or folded. The nasal bones might require shaving or infracturing. Cartilage grafts may be required as well. The incisions are then closed and a nasal splint is applied. Sometimes nasal packing is used to eliminate drainage and seal the tissues together. Some patients’ surgeries are more involved than others, and if there are breathing issues this adds to the surgical time. Rhinoplasties requiring extensive septal work or secondary revision rhinoplasty will often take longer.
Recovery
During rhinoplasty recovery, you will have a nasal splint and may have nasal packing inside your nose. The packing is often removed within one or two days, and the nasal splint often is removed within one week. If there are external sutures, these are often also removed at this time. You will likely have bruising and swelling throughout the nose and face. Most bruising will go away within one to two weeks. Within two weeks, you should be able to return to most activities, but please wait another four to six weeks before resuming vigorous exercise. The majority of swelling will go down in six to eight weeks but the nose may still stay slightly swollen for a year or longer. Use extra pillows to keep your head elevated when resting on your back. We’ll schedule regular follow-up appointments to monitor your progress.
Results
Once your symptoms are resolved, you will be able to enjoy the long-term benefits of an enhanced nasal shape and function.
Cost of Rhinoplasty in New York City
Rhinoplasty surgeries deliver customized results, and accordingly, your final price is based on your personalized treatment plan devised by Dr. Wallach. Depending on your treatment plan, your rhinoplasty surgery may cost anywhere from $7,500 – $40,000. These costs may include things like general anesthesia, tests, surgical facility costs, and more. In some cases, patients with respiratory concerns may have their surgery covered by their insurance. Financial matters will be discussed in-depth following your personal consultation. We encourage patients to explore our financing options.
References
- Gupta P, Tripathi T, Singh N, Bhutiani N, Rai P, Gopal R. A review of genetics of nasal development and morphological variation. Journal of Family Medicine and Primary Care. 2020;9(4):1825-1833. doi:10.4103/jfmpc.jfmpc_1265_19
- Rohrich RJ, Ahmad J. Rhinoplasty. Plastic and Reconstructive Surgery. 2011;128(2):49e73e. doi:10.1097/prs.0b013e31821e7191
- Deroee AF, Younes AA, Friedman O. External nasal valve collapse repair: the limited alar-facial stab approach. The Laryngoscope. 2011;121(3):474-479. doi:10.1002/lary.21410
- Gagnieur P, Fieux M, Louis B, Béquignon E, Bartier S, Vertu Ciolino D. Objective diagnosis of internal nasal valve collapse by four phase rhinomanometry. Laryngoscope Investigative Otolaryngology. 2022;7(2):388-394. doi:10.1002/lio2.784
- Godin MS, Waldman SR, Johnson, Jr CM. Nasal Augmentation Using Gore-Tex. Archives of Facial Plastic Surgery. 1999;1(2):118-121. doi:10.1001/archfaci.1.2.118